 |
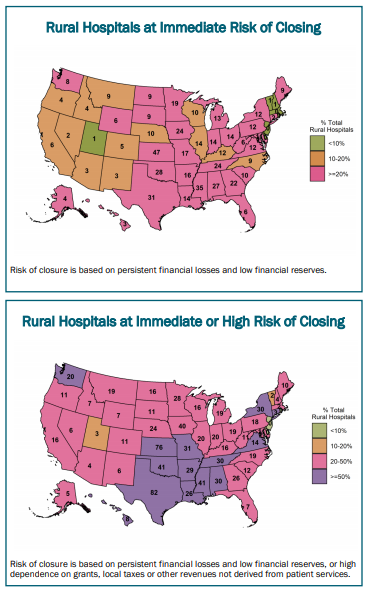
| Maps from "Rural Hospitals at Risk of Closing" report |
You can get a pretty good idea from an analysis and a database published by the Center for Healthcare Quality and Payment Reform, a research center chartered by Congress.
The center's report doesn't name the at-risk hospitals, but it does offer a wealth of financial information about most of the short-term, acute-care hospitals in rural America.
Harold Miller, president and CEO of the center, told Melissa Patrick of Kentucky Health News that the report doesn't name the hospitals the center considers at risk because it's hard to say exactly what is going on in each of them without digging a bit deeper into their individual stories, and he doesn't want to imply that the only hospitals struggling are the ones he puts on a list.
"This was more intended to say to the state, 'Guess what, you have a bunch of hospitals that are not doing well and you shouldn't ignore that problem'," he said.
Harold Miller, president and CEO of the center, told Melissa Patrick of Kentucky Health News that the report doesn't name the hospitals the center considers at risk because it's hard to say exactly what is going on in each of them without digging a bit deeper into their individual stories, and he doesn't want to imply that the only hospitals struggling are the ones he puts on a list.
"This was more intended to say to the state, 'Guess what, you have a bunch of hospitals that are not doing well and you shouldn't ignore that problem'," he said.
An earlier report rom the Chartis Group, a rural-health consultancy, says 135 rural hospitals have closed since 2010, and 453 more are vulnerable to closure.
The new "Rural Hospitals at Risk of Closing" report says hospitals with an immediate risk of closing have had persistent financial losses, meaning "the hospitals had a cumulative negative total margin over the most recent three-year period for which financial data were available" and had a low or non-existent financial reserve, meaning the hospitals either "had total liabilities exceeding all assets other than buildings or equipment or had assets greater than liabilities, but only by enough to sustain continued losses for at most two years."
The report says the primary cause of rural hospital closures is that payments from government and private health-insurance plans is less than the cost of delivering care to patients in rural communities; that these payments are not enough to sustain their essential services.
Rural hospitals' financial troubles are often blamed on low reimbursement from Medicare and Medicaid, but Miller said some small rural hospitals have more trouble with private health plans, which pay them less than big hospitals for the same care, and less than the cost of delivering that care.
"It's not as if there is just one thing that explains why they're losing money," Miller said. "In some cases, it's more Medicaid patients, in some cases, it's bad payments by commercial payers. In some cases, and it's hard to tell that from these data, it's sometimes the mix of services that hospital offers."
The report shows the payer mix of hospitals and what they make or lose on patient services in addition to their total margins. It reviews many of the problems faced by rural hospitals and analyzes many of the proposed solutions, and offers a new approach.
It proposes a two-part payment model that would require an up-front payment from both public and private insurers based on the number of plan members who live in the community, regardless of the number of services provided, along with a service-based fee much lower than current payment models.
This "patient-centered payment system" would ensure "that the hospital has adequate revenues to support the minimum standby costs of essential services, such as the emergency department, inpatient unit and laboratory," and the service fee "would ensure that if patients need more services, the hospital would receive sufficient additional revenue to cover the added costs of delivering those services, rather than being forced to delay or ration care," the report says.
This "patient-centered payment system" would ensure "that the hospital has adequate revenues to support the minimum standby costs of essential services, such as the emergency department, inpatient unit and laboratory," and the service fee "would ensure that if patients need more services, the hospital would receive sufficient additional revenue to cover the added costs of delivering those services, rather than being forced to delay or ration care," the report says.
"We need to do something different," Miller told Kentucky Health News. "All the stuff we've tried so far hasn't worked."
No comments:
Post a Comment